Overview
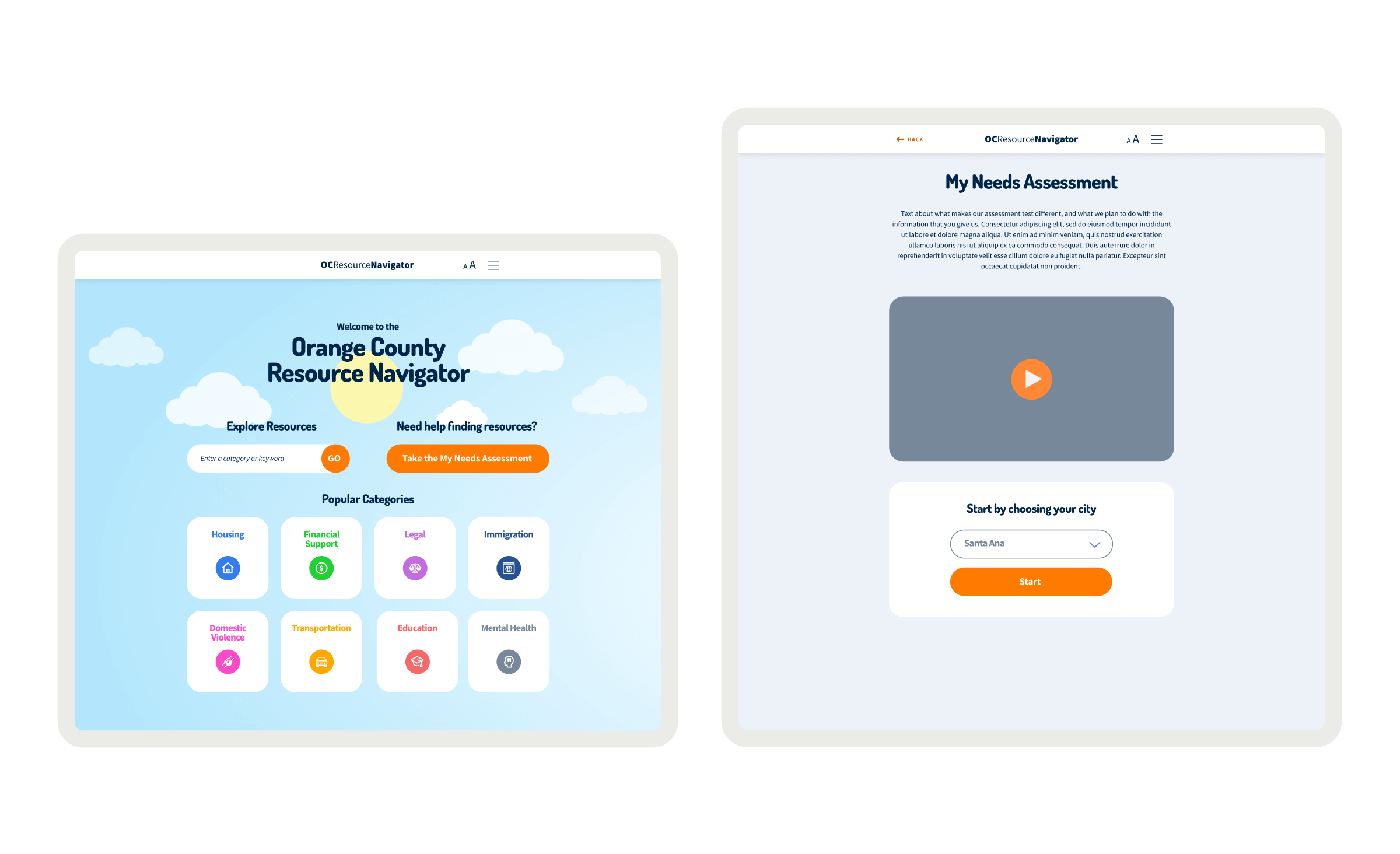
The OC Navigator digital platform improves how Orange County residents connect with mental health resources by recognizing how physical, mental, and social health interact. By acknowledging that traditional resource navigation is fractured, confusing, and often inaccessible, the platform empowers individuals and providers to find appropriate services through a human-centered approach. Through stakeholder collaboration, social determinants of health screening, and culturally responsive design, the experience design helps bridge the gap between need and service for the 20.7% of Orange County adults who report needing mental health support.
Research & Design
Participatory Design Research · UX & UI Design · Accessibility & Privacy Compliance · Prototyping · Journey Mapping User Research · Stakeholder Collaboration
- Duration: February-July 2022
- Partners: CalMHSA, Orange County Health Care Agency, UCLA
- Team: Fas Lebbie, Kris, Bowen Chung, Minhxuan Tran
Confidentiality: Details have been adapted to protect sensitive information while showcasing my design approach.

What I Brought
I led co-design sessions and structured interviews with community members, providers, and stakeholders, turning lived experiences into actionable insights that guided implementation of ecosystem mapping and journey frameworks to drive $18 million transformation initiative outcomes, as well as the platform’s design.
I translated complex healthcare needs into clear, accessible mobile and web interfaces, embedding WCAG and HIPAA-aligned practices into design decisions.
Problem Context
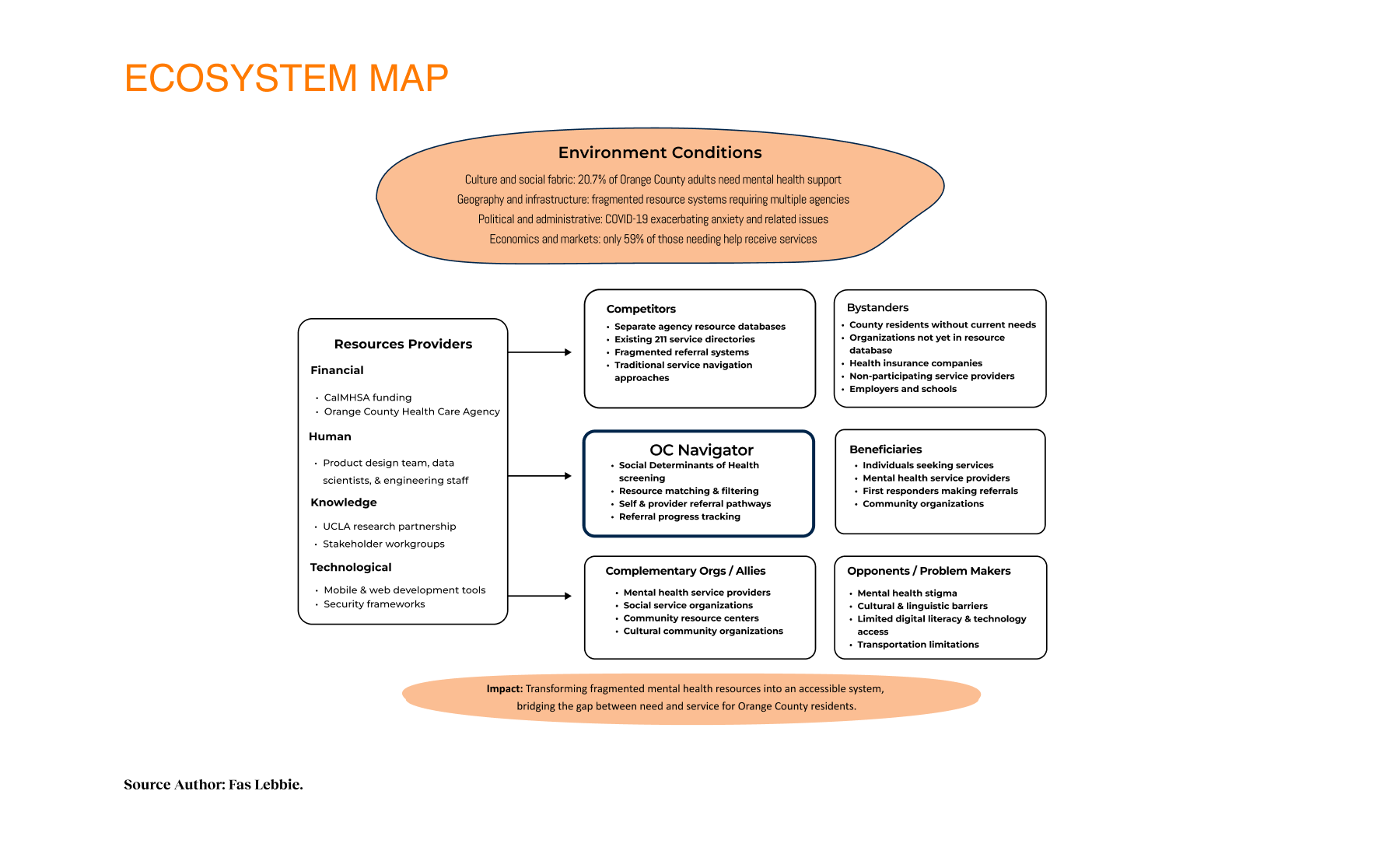
In Orange County, 20.7% of adults need help with mental health or substance abuse issues, but only 59% receive the care they need. This disparity highlights a significant gap in mental health resource access, especially for diverse communities. COVID-19 worsened these challenges, increasing anxiety, isolation, and social issues like housing and food insecurity. Resource hubs have gone virtual, intensifying barriers such as transportation, linguistic and cultural obstacles, and mental health stigma. The fragmented resource navigation system required navigating multiple agencies, repeating stories, and meeting complex eligibility requirements. Public and private behavioral health systems lack coordination, and insurance networks often fail to support person-centered access and service delivery. Current care models focus on quantity-based measures over recovery-oriented outcomes, creating a disconnect between services and user needs. This fragmentation mainly affects vulnerable populations with limited English proficiency, technology access, or health literacy. Service providers maintain separate resource databases, causing confusion and missed care opportunities. By connecting people with the resources they need, there is an opportunity to create a more inclusive, responsive system that reduces barriers and enhances access to mental health support. The Navigator addresses this challenge by focusing on individual journeys rather than isolated system touchpoints.
My Approach
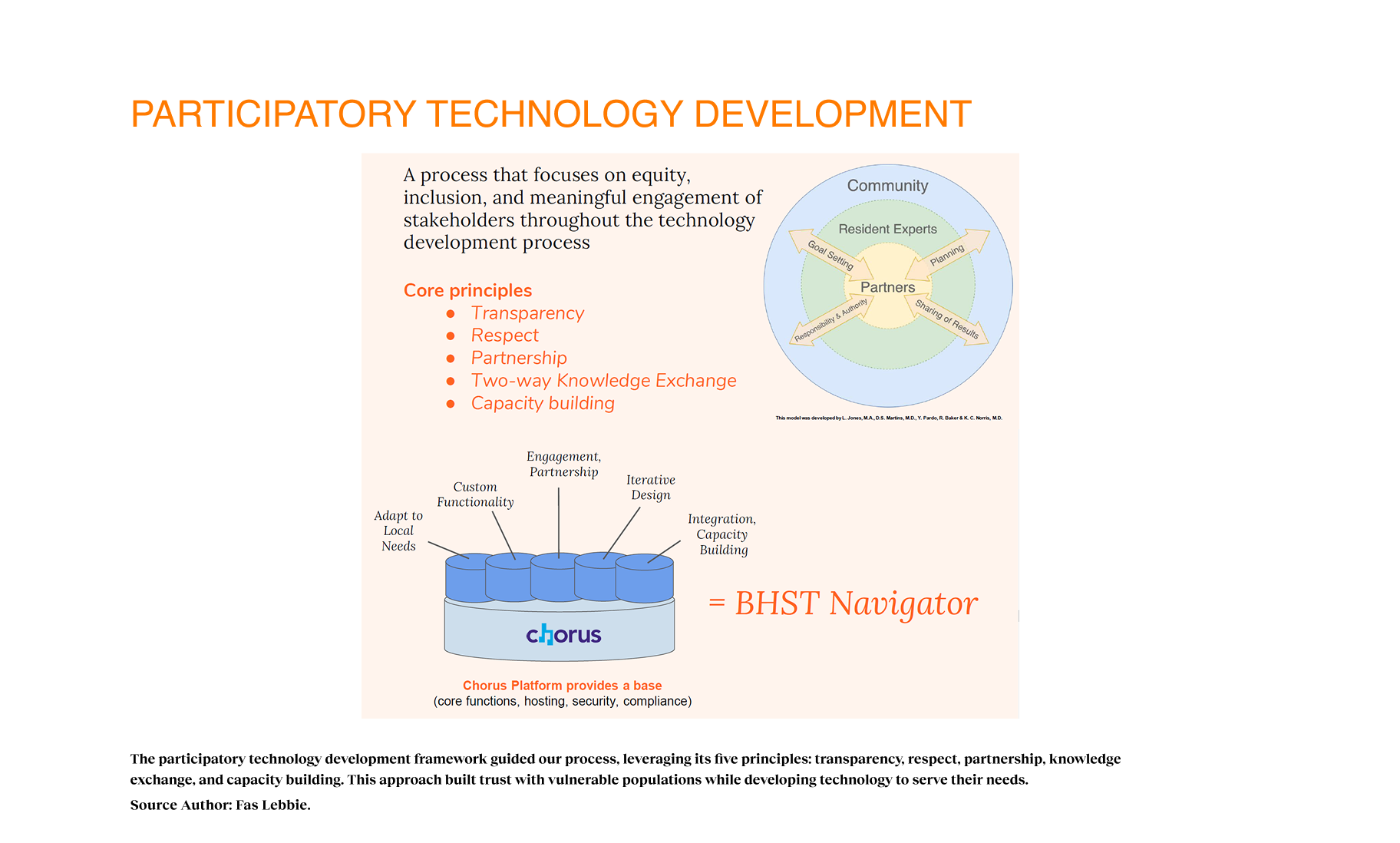
My approach centered on participatory technology development, a process that focuses on equity, inclusion, and meaningful engagement of stakeholders throughout the technology development process. My design process integrated core values of transparency, respect, partnership, two-way knowledge exchange, and capacity building. By engaging diverse stakeholders as partners in the development cycle, we ensured the technology responded to local needs.
Design Process
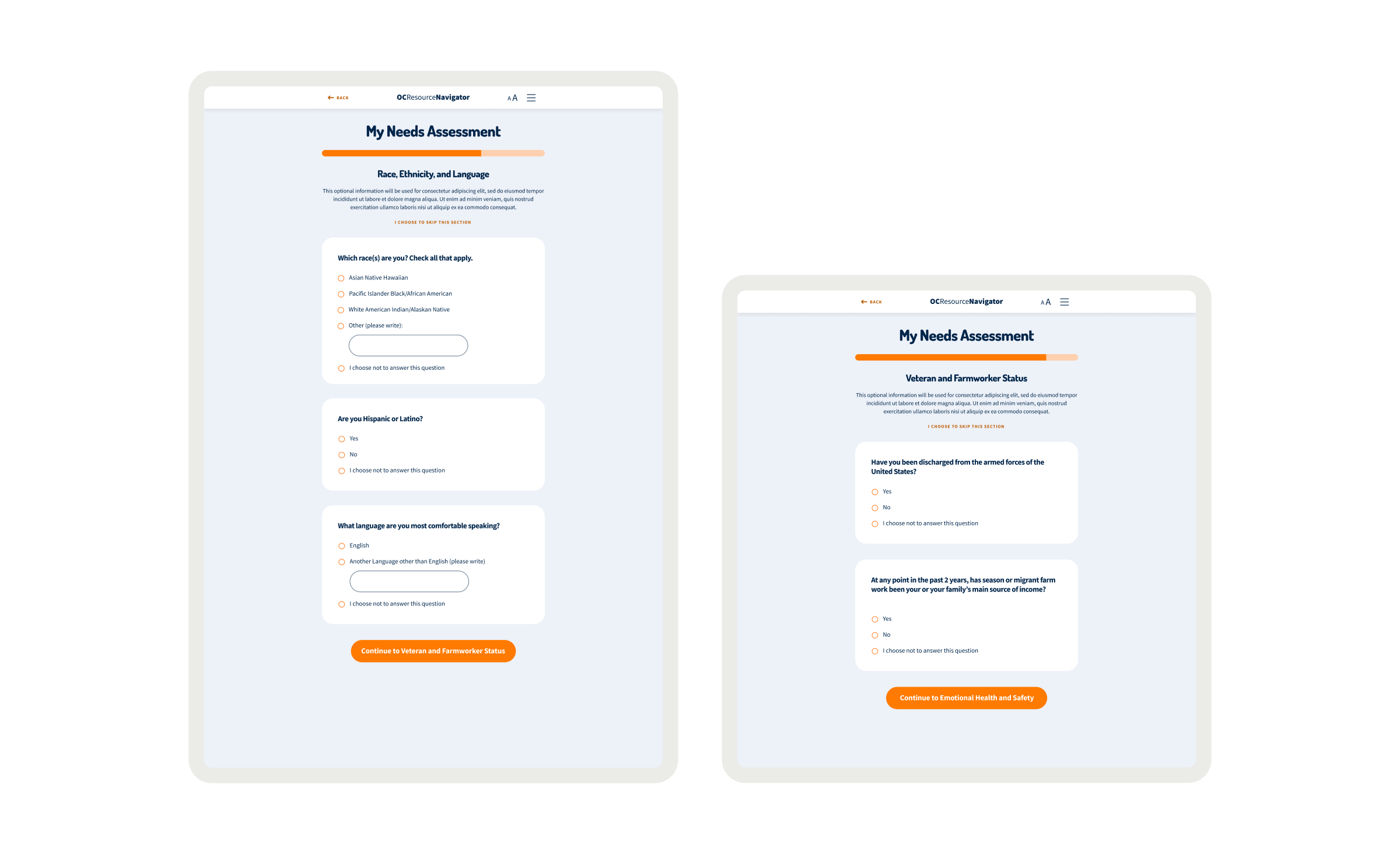
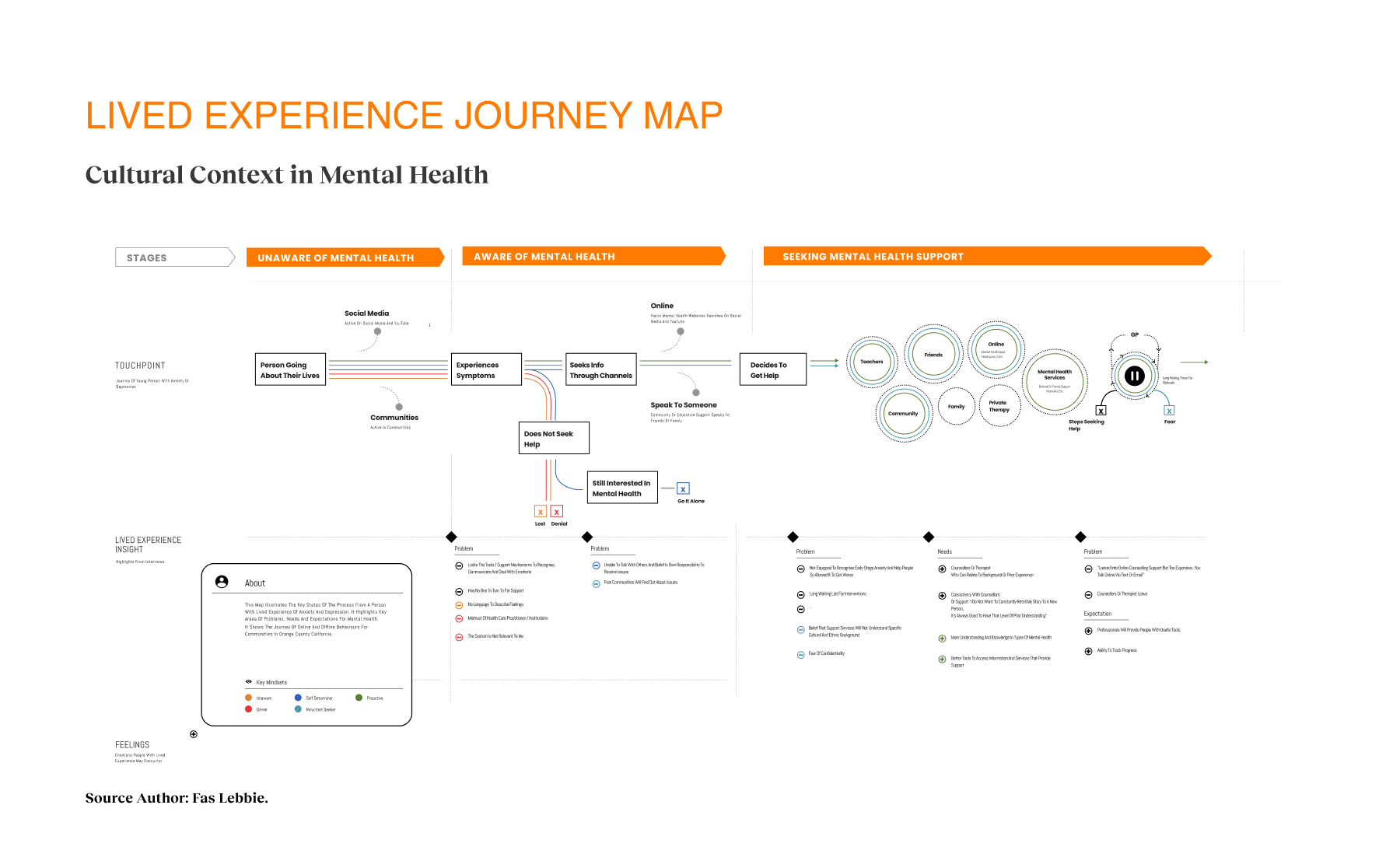
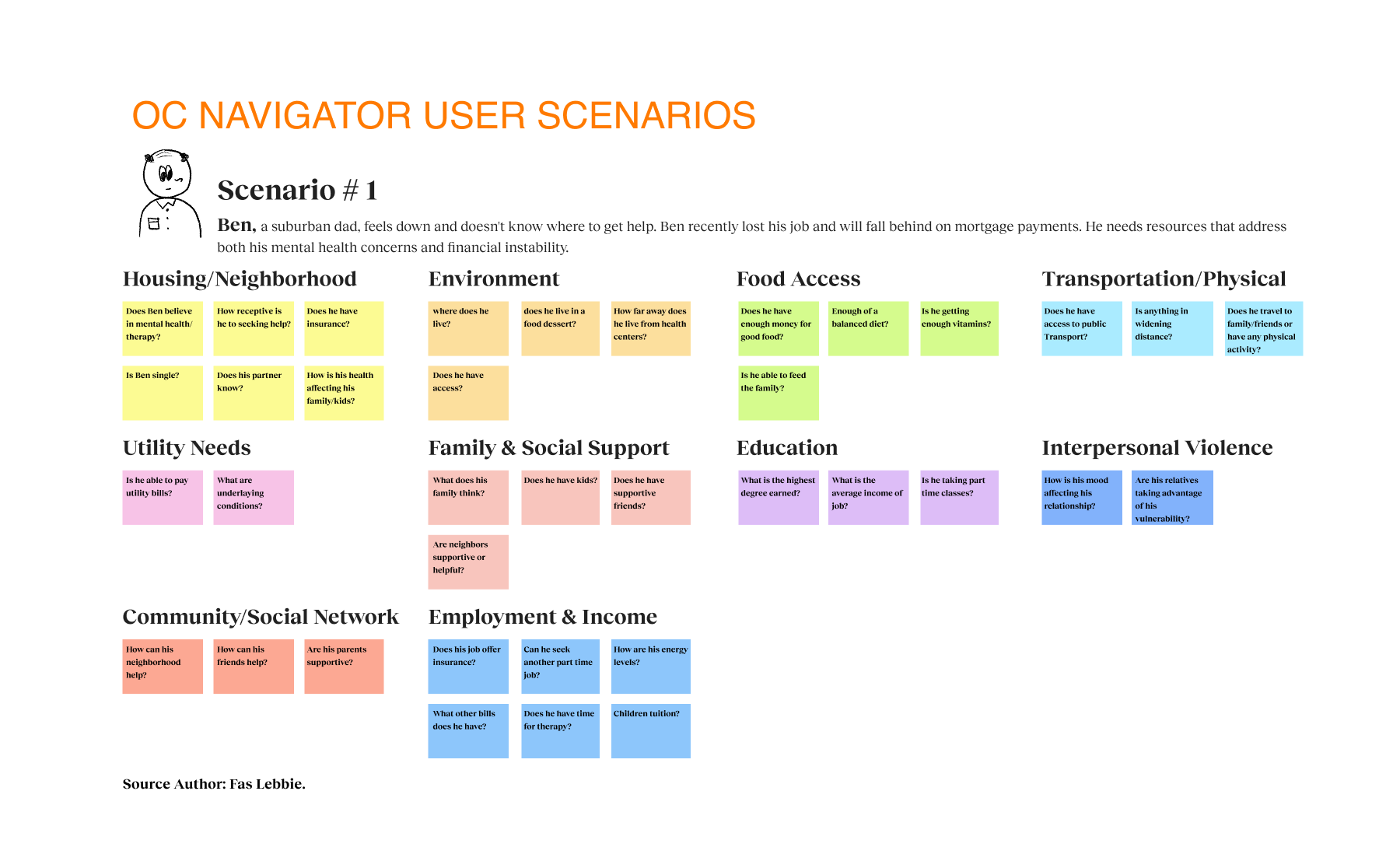
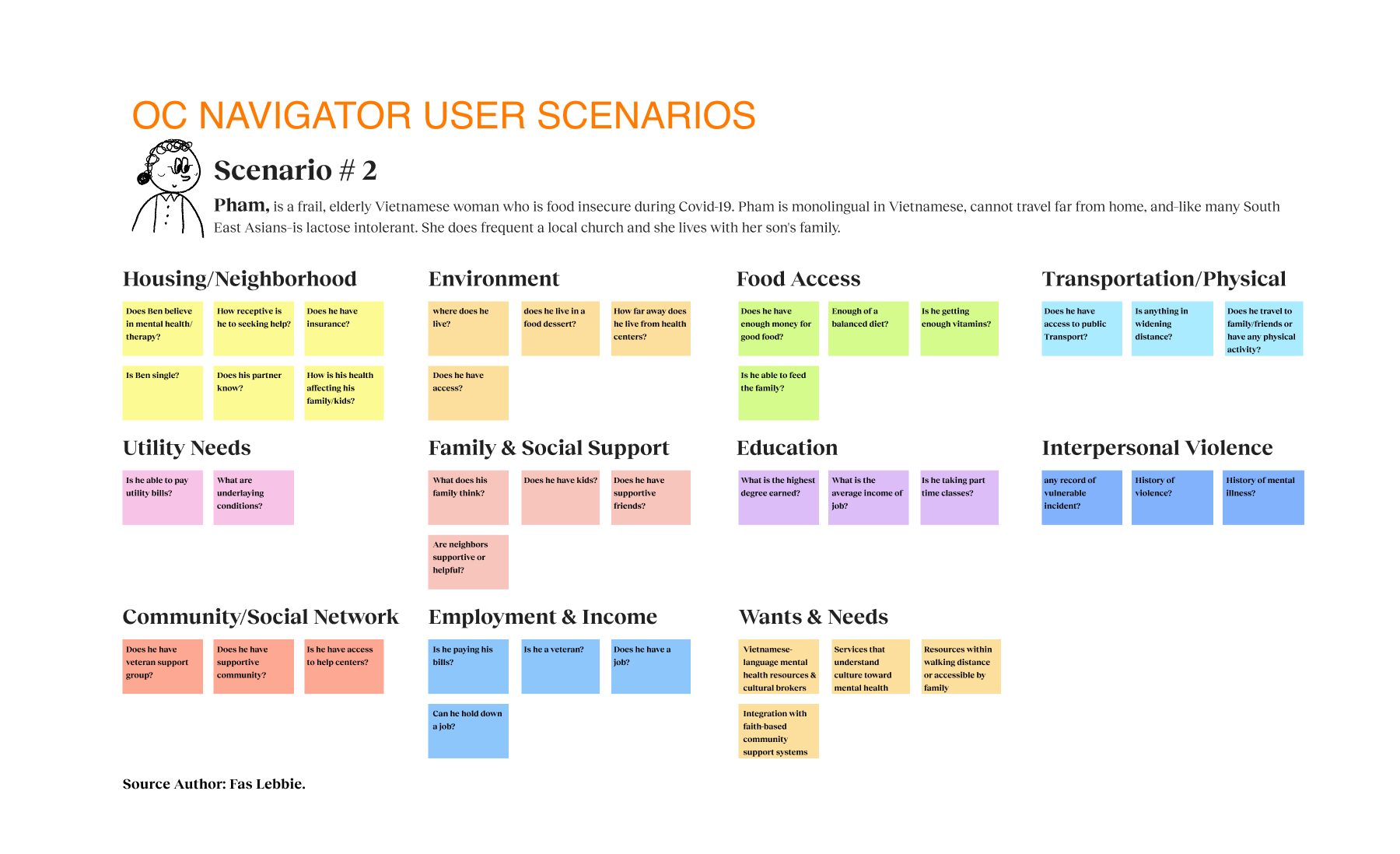
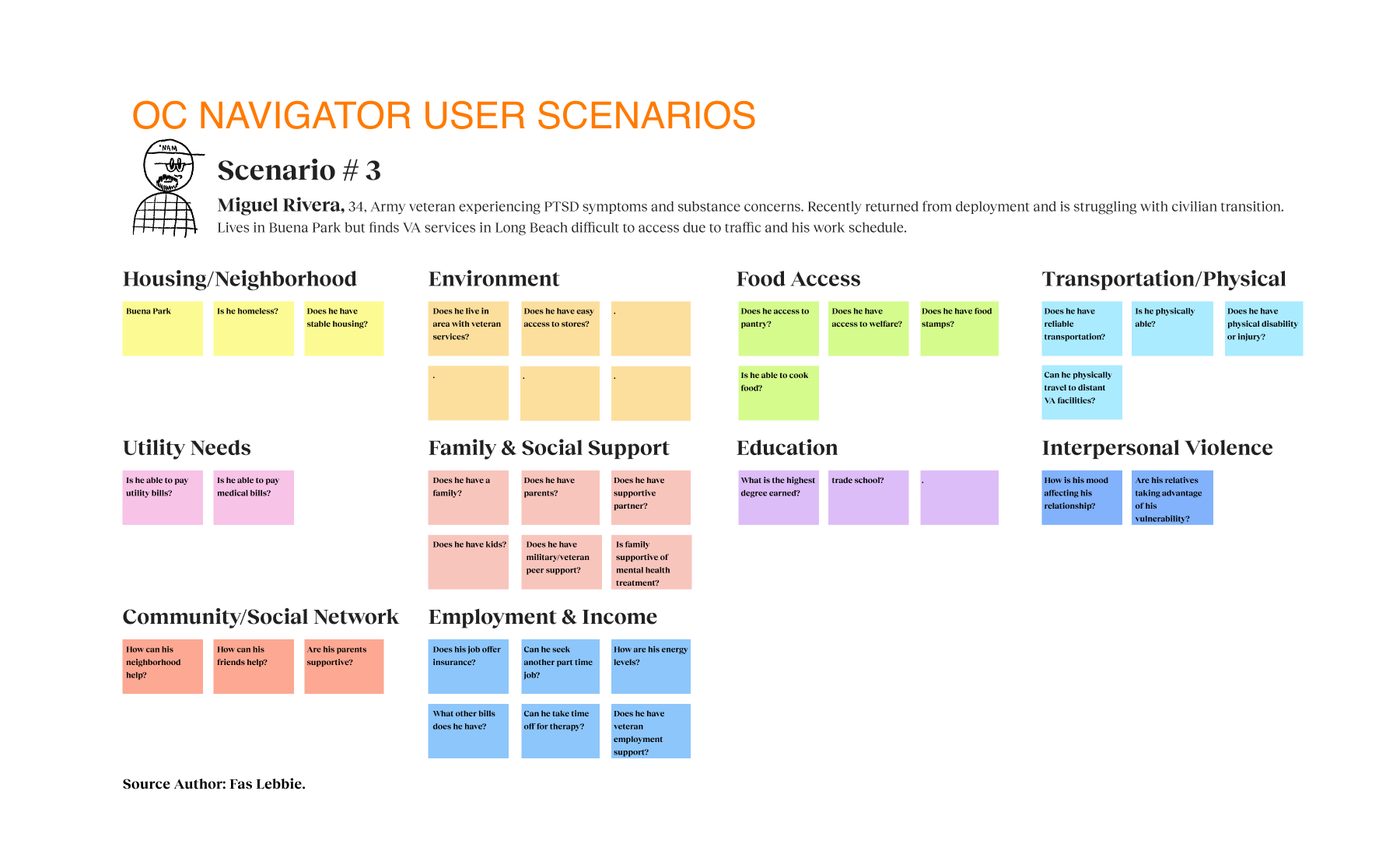
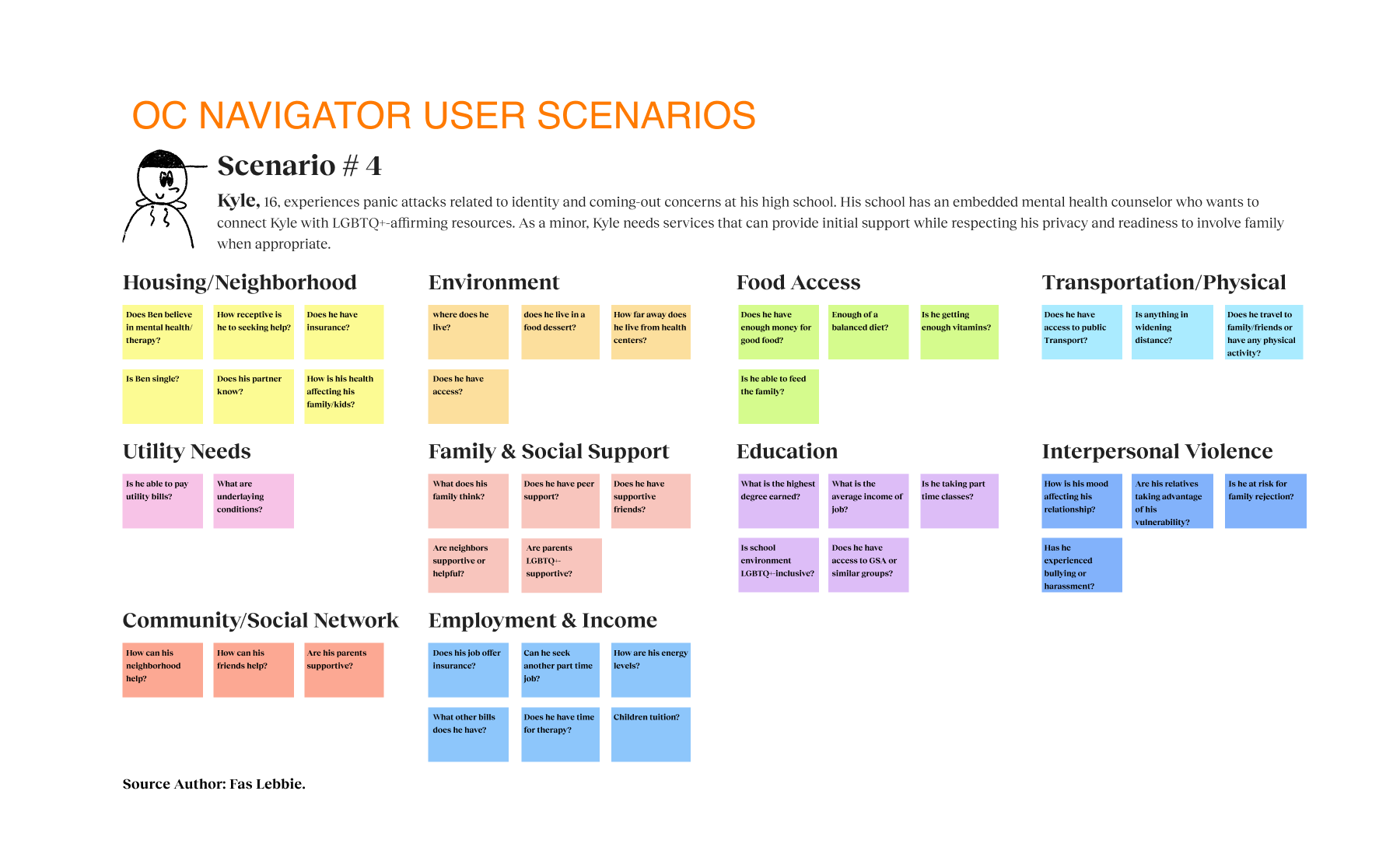
Before I joined, the Chorus team conducted focus groups and workshops, providing me with valuable data. This data allowed us to make informed, data-driven decisions that enhance engagement. Their research revealed one in five adults needs help with mental, emotional, or substance abuse issues. The team also examined how traditional resource navigation often fails to serve diverse populations, especially those facing linguistic barriers, limited technology access, or complex social determinants that affect their health. Additionally, I learned that geographic location, insurance status, and service eligibility criteria pose significant challenges, while cultural stigma often discourages individuals from seeking assistance. In response to these systemic barriers, I based our research on the realities faced by those most affected, particularly monolingual communities, older adults, and individuals with limited digital literacy.
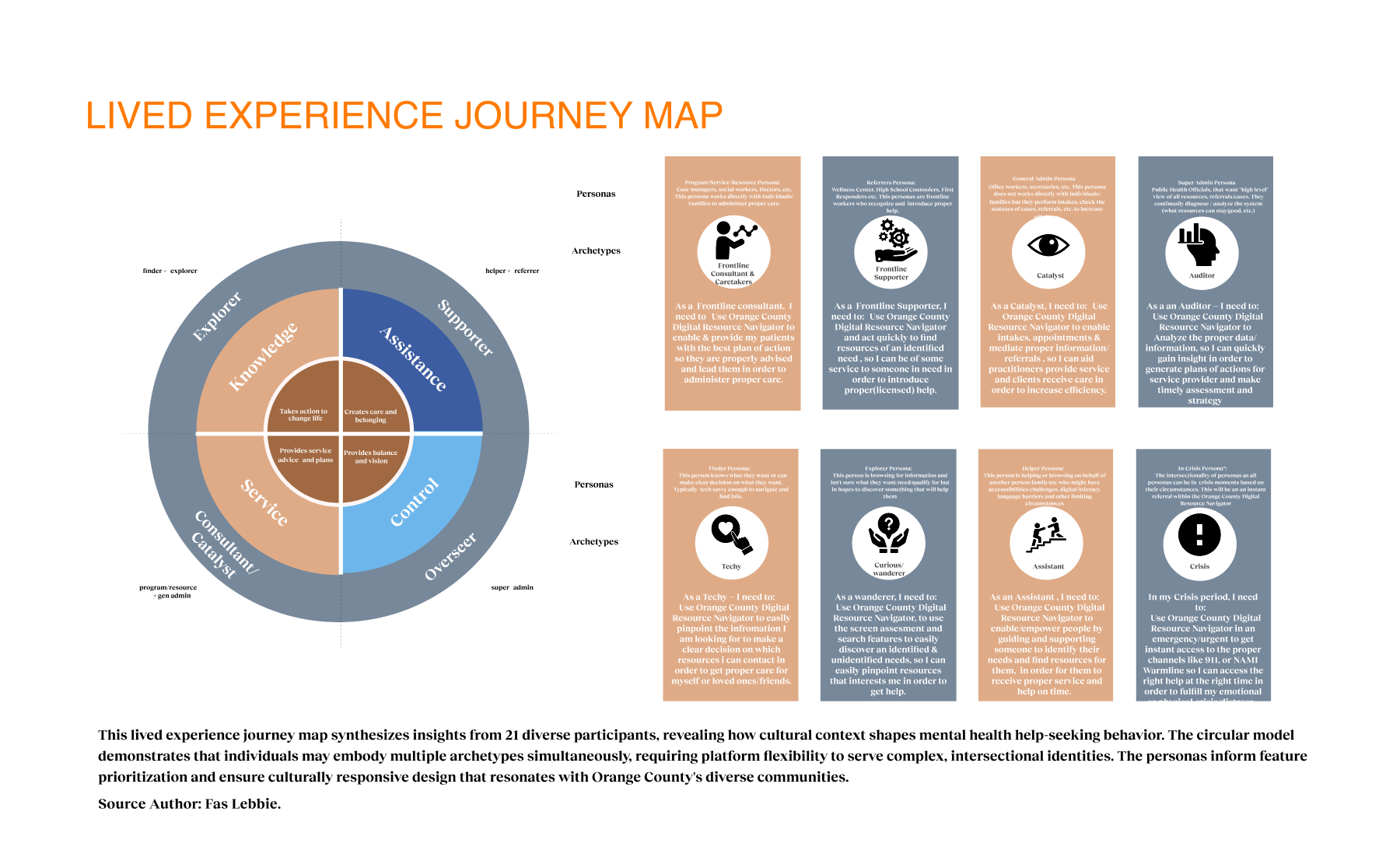
I used the grounded theory approach, conducting structured and semi-structured interviews with eight stakeholders and four workgroups, totaling 21 participants, to explore mental health resource navigation challenges. We engaged with a diverse group of participants, including first responders, community organization leaders, program administrators, and citizens, to capture multiple perspectives. Each 30 to 90-minute session uncovered personal stories that highlighted key insights about the resource journey.
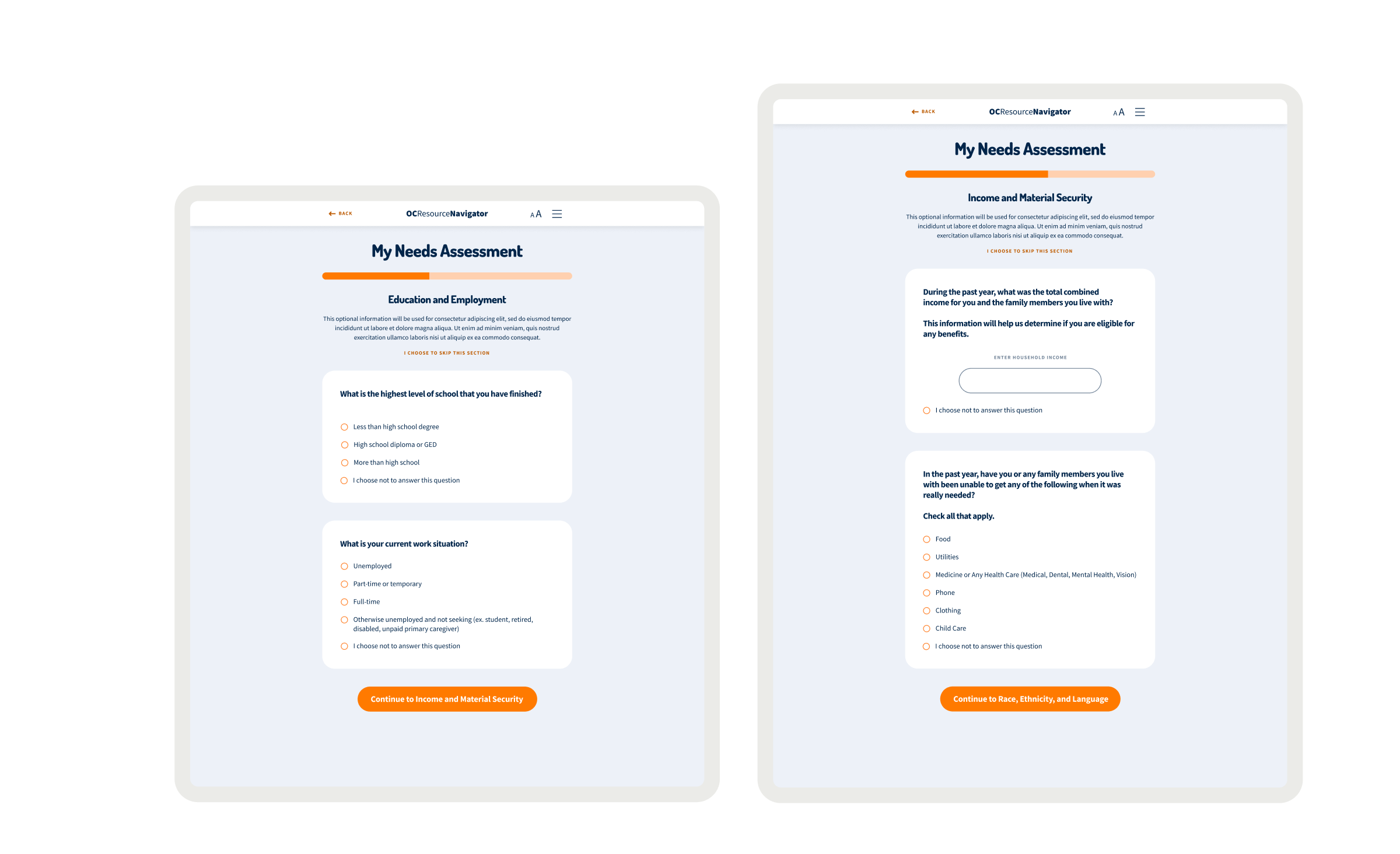
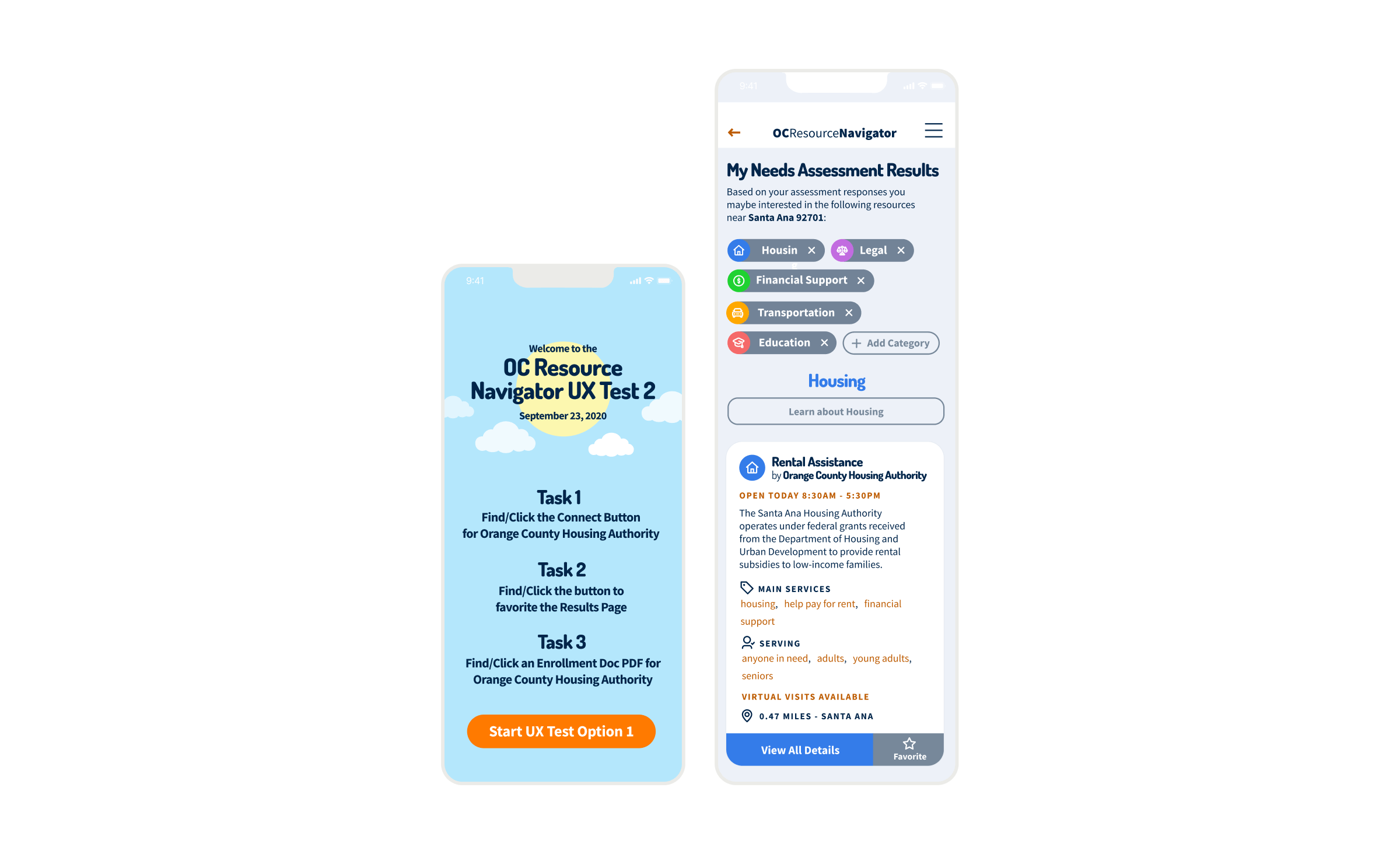
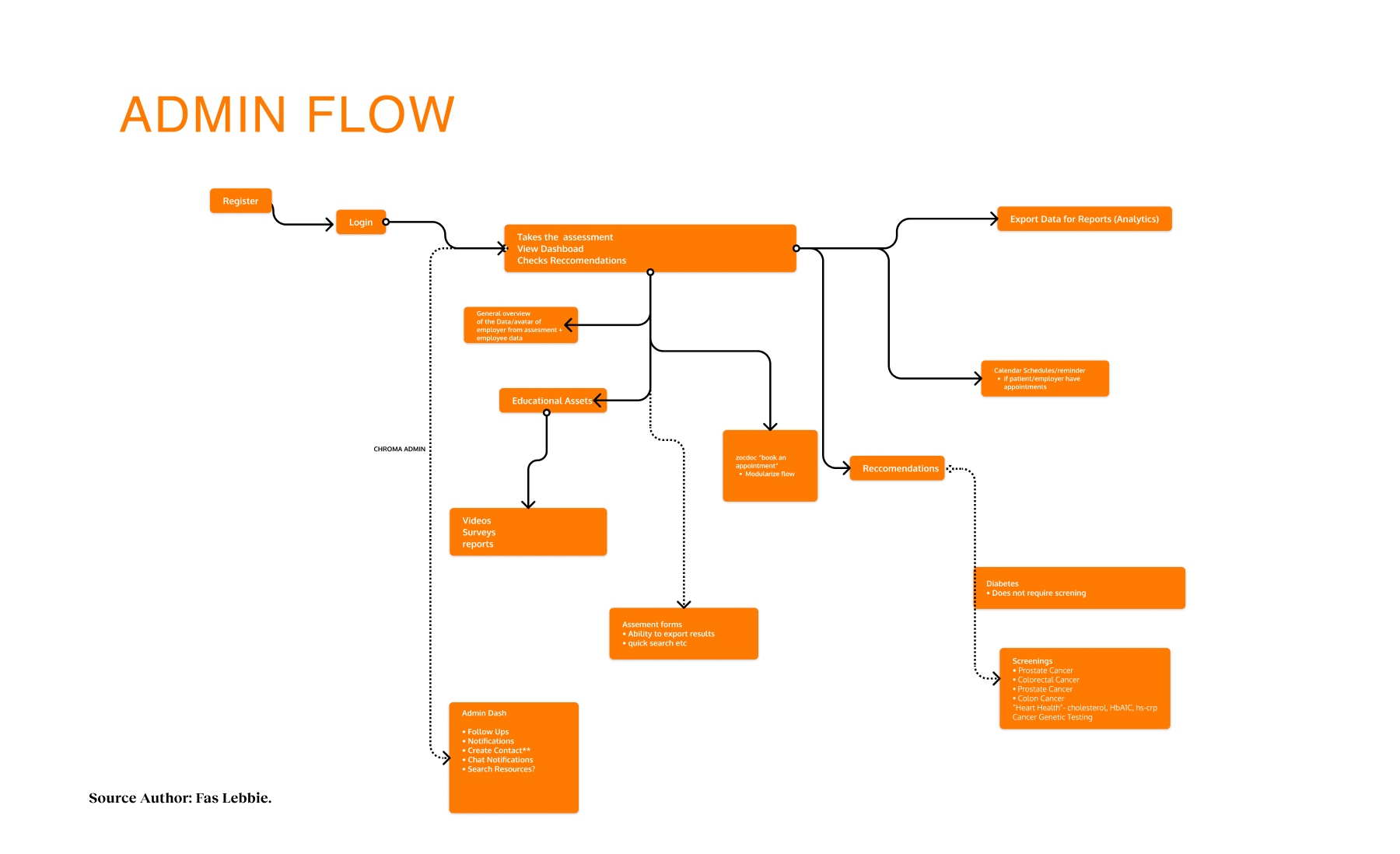
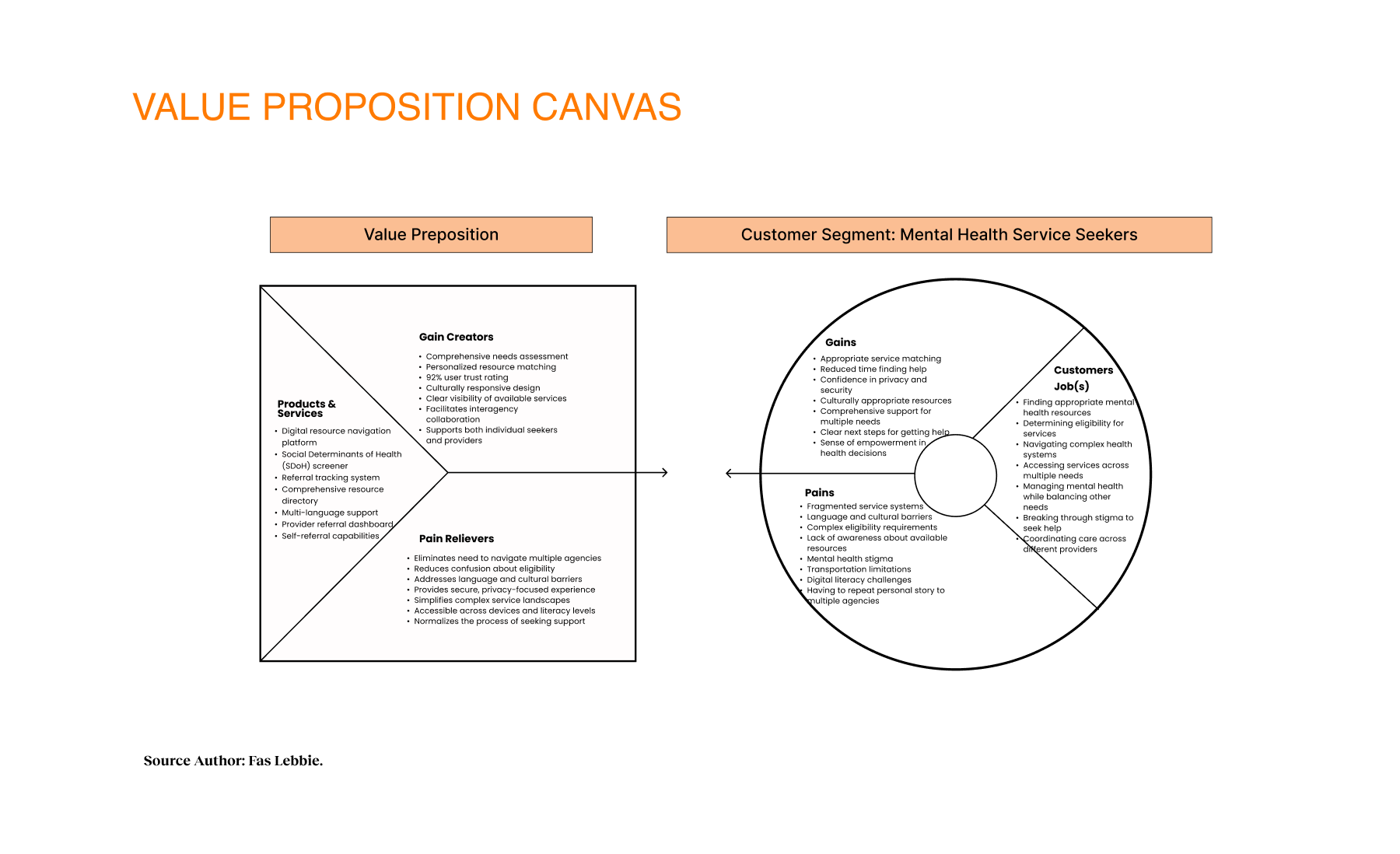
The research identified opportunities to bridge the gap between mental health needs and resource access. Participants reported significant barriers to finding appropriate services, such as lack of awareness, cultural and linguistic obstacles, and transportation challenges. Trust was critical for successful resource navigation, with 92% of participants emphasizing service transparency. Social determinants like housing stability, food security, and social support networks significantly affected access to mental health services. These insights presented design intervention opportunities for those struggling with mental health challenges who lack the knowledge, resources, or support to navigate complex systems. We proposed a digital platform with two user journeys — one for individuals seeking services and another for providers making referrals. The MVP was built on three requirements:
- The design must incorporate best practices for usability and accessibility in mental health service navigation.
- The platform must integrate a social determinants of health screener to capture needs and connect them with resources.
- The design must ensure data security and privacy while maintaining ease of use to foster trust and encourage adoption.
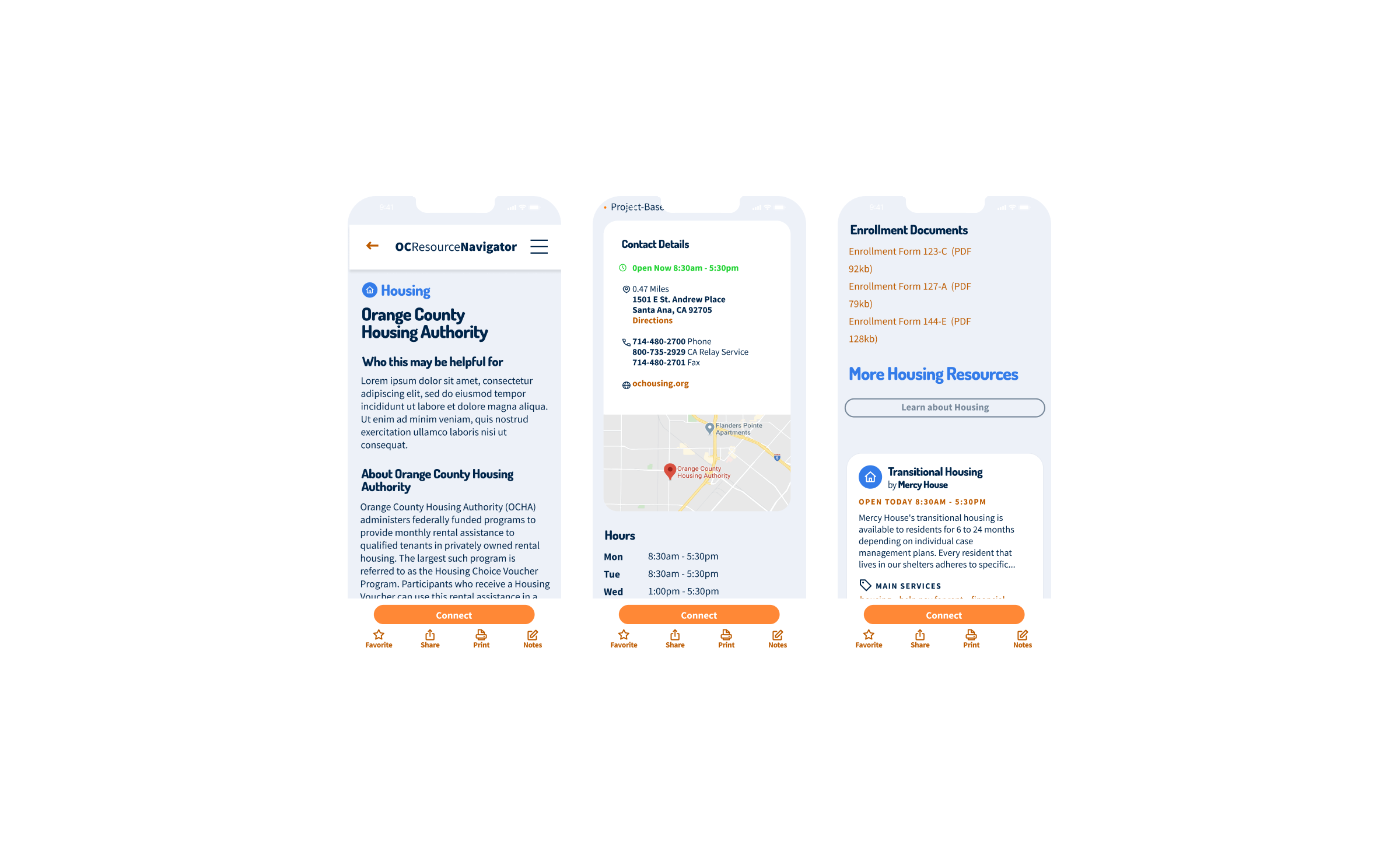
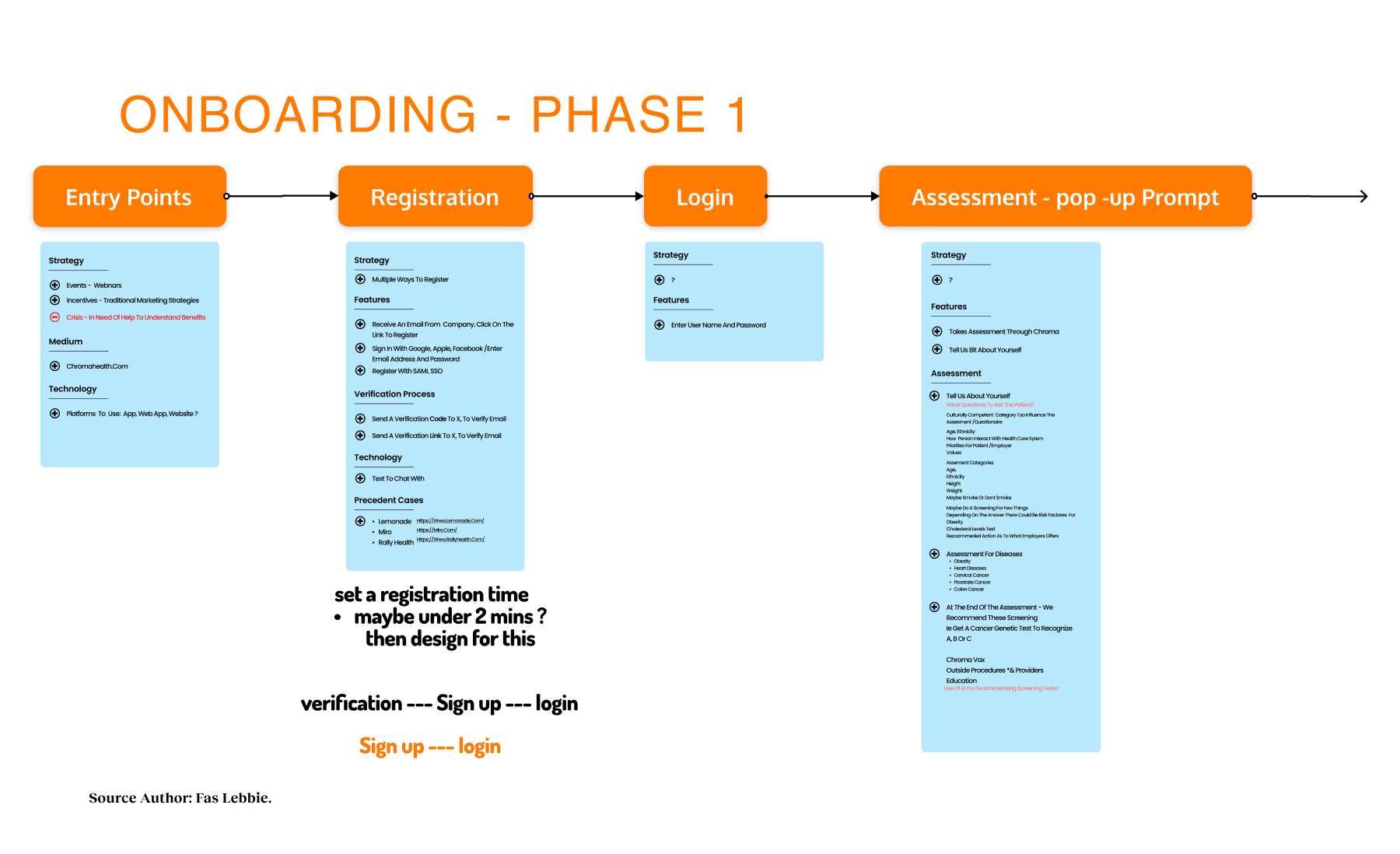
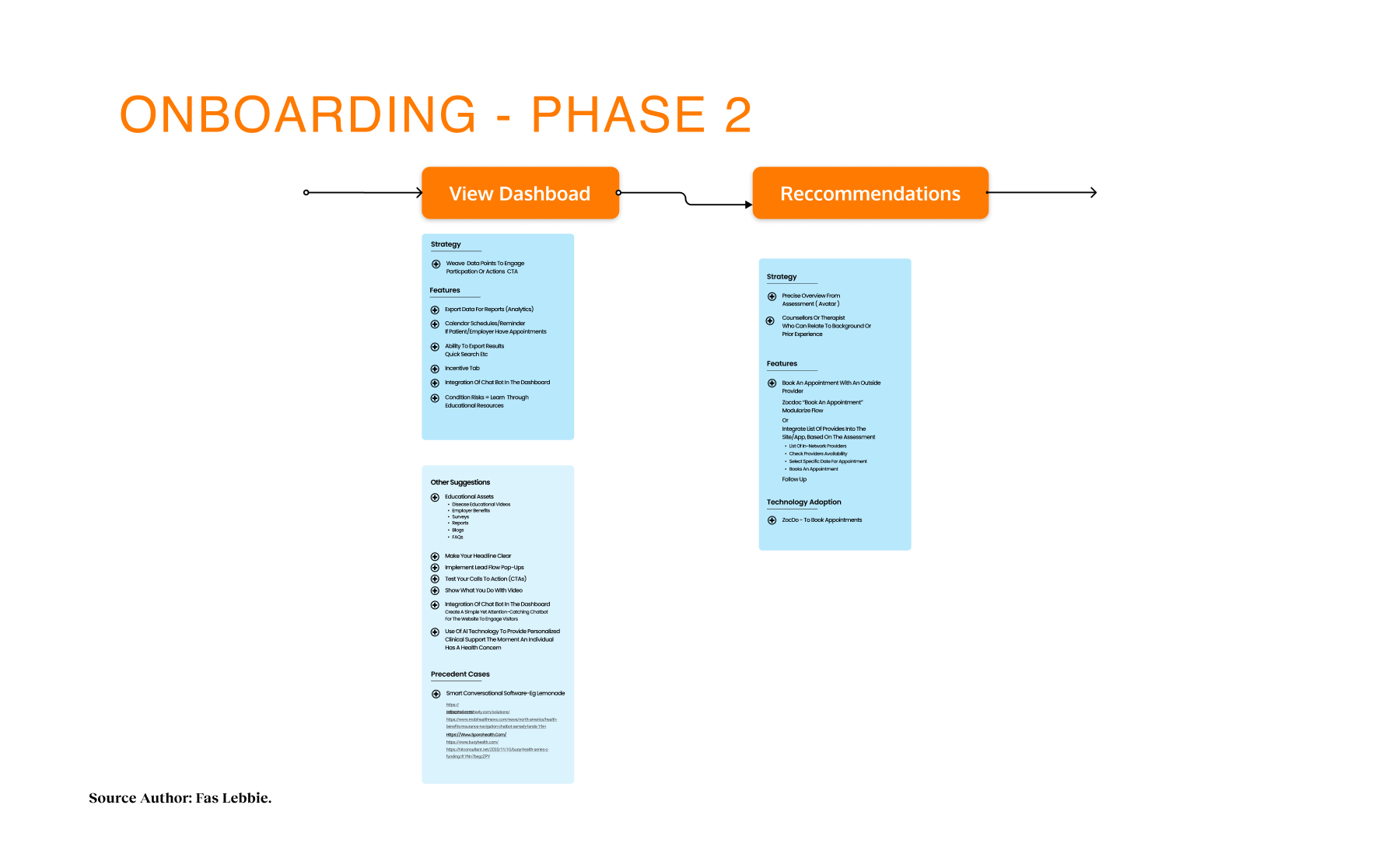
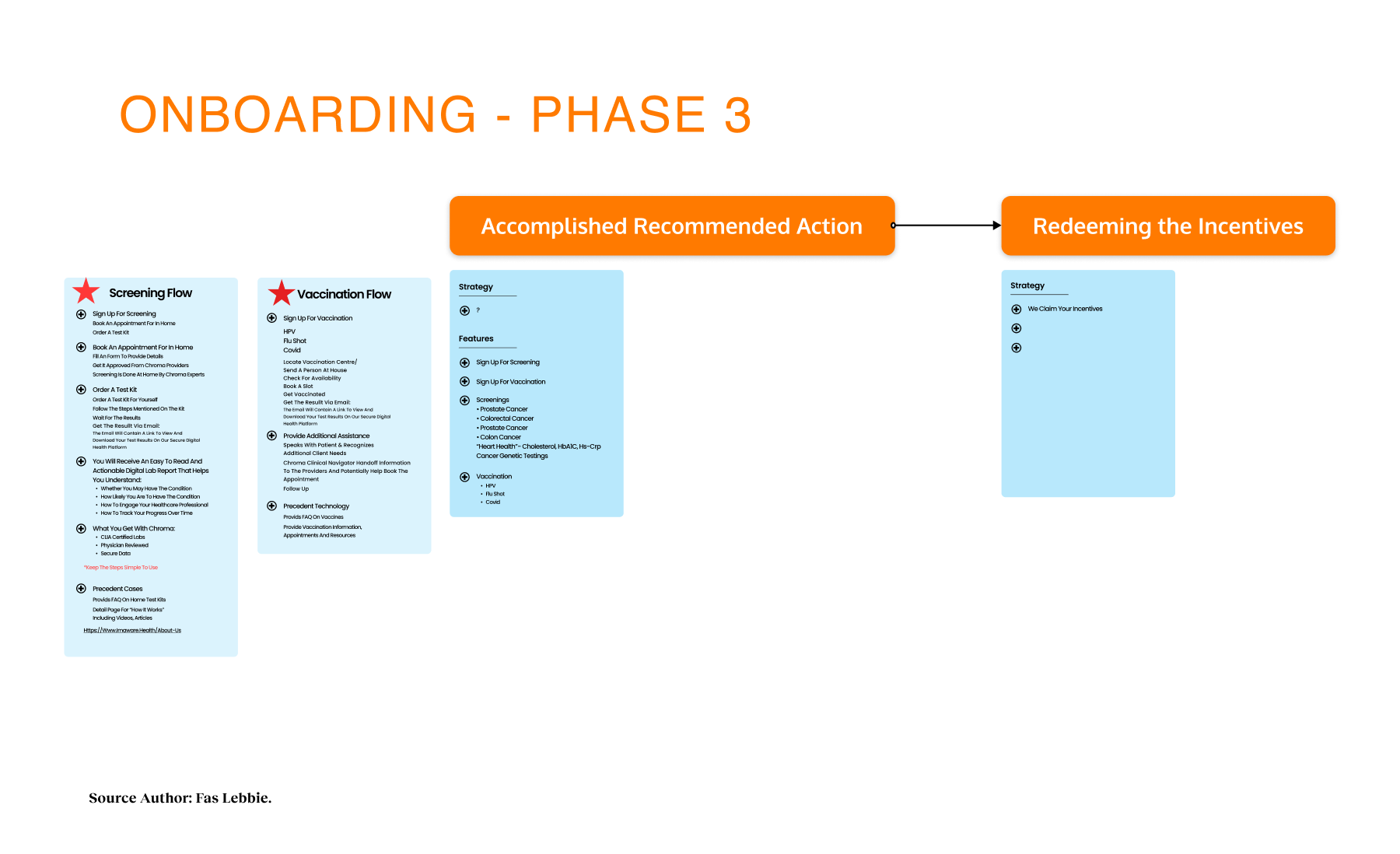
Prior to the build phase, an initial version was deployed for testing. The v1.0 pilot was scheduled for March 2021, with iteration, improvement, and scaling continuing through June 2022. AB testing was done through specific user and additional stakeholder interviews, and journey mapping was conducted through feedback loops from testing sessions as well as during the development process. Implementation focuses on core functionality for individual users, including the home page, social determinants screener, and basic resource listings, before expanding to the provider dashboard and referral tracking system. Each phase incorporated user feedback, particularly around privacy concerns and progress visibility.
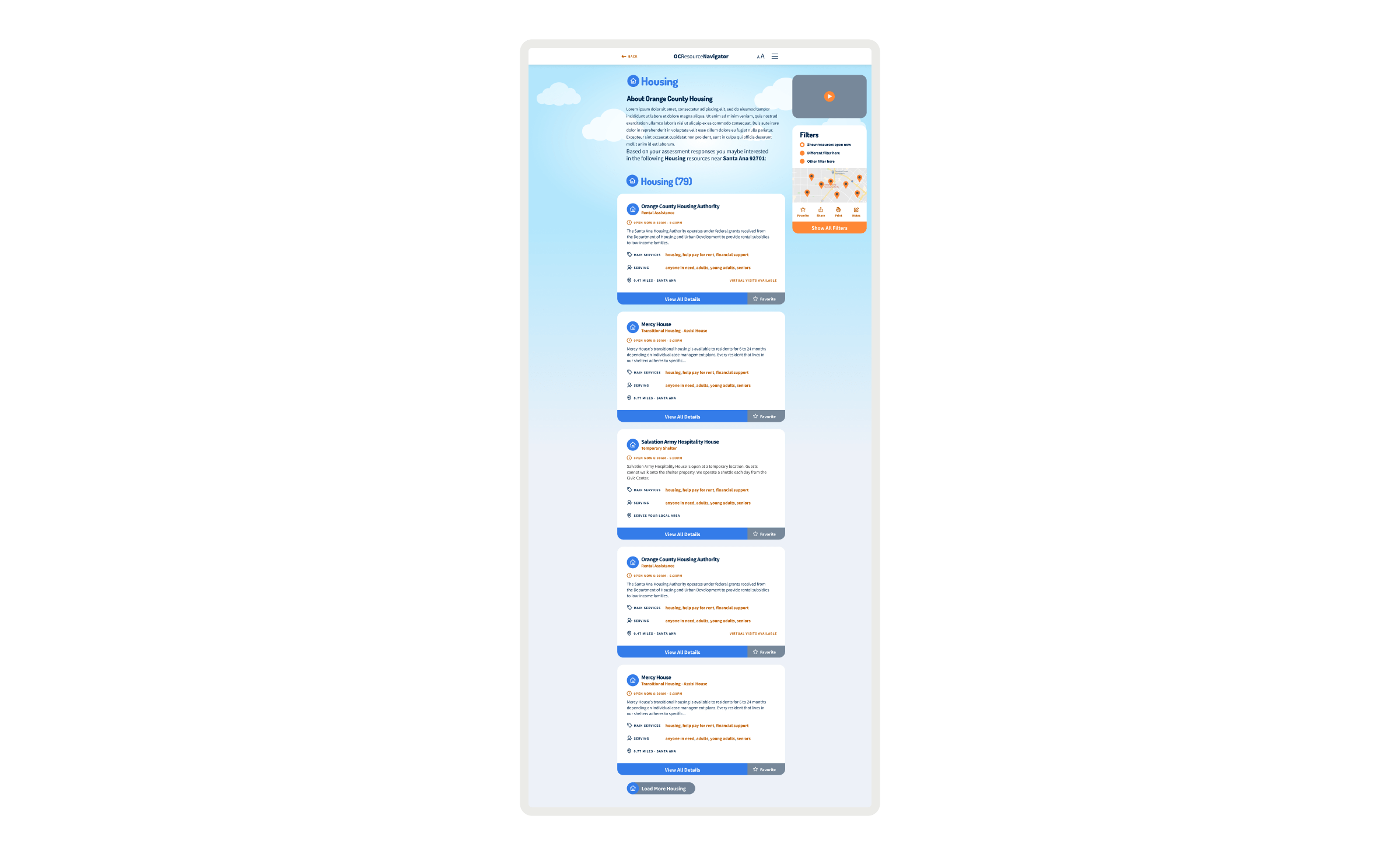
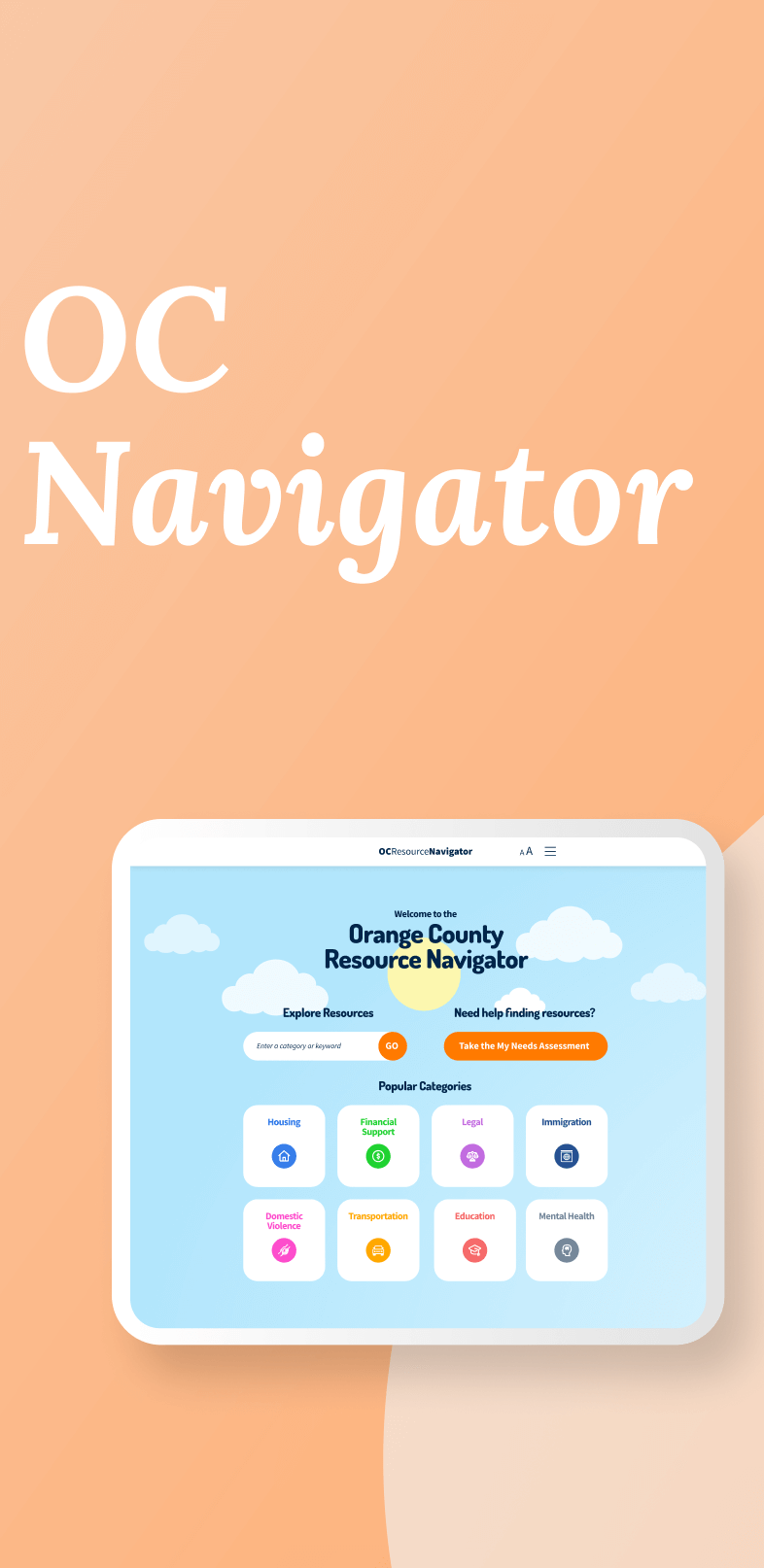
Connecting residents to mental health and social services with lists of resources for different needs and topics, focusing on trust, accessibility, and culturally responsive design.
Individual

Social Worker

Office Admin

Service provider

Navigation Adoption
71% of patients offered navigation choose to receive help, guiding uptake targets.
Increase In Referral Completion
Represents over 650,000 residents requiring mental health services, demonstrating the massive scale of need addressed by the platform.
Orange County Adults Needing Support
Represents over 650,000 residents requiring mental health services, demonstrating the massive scale of need addressed by the platform.
Reflections & Impact
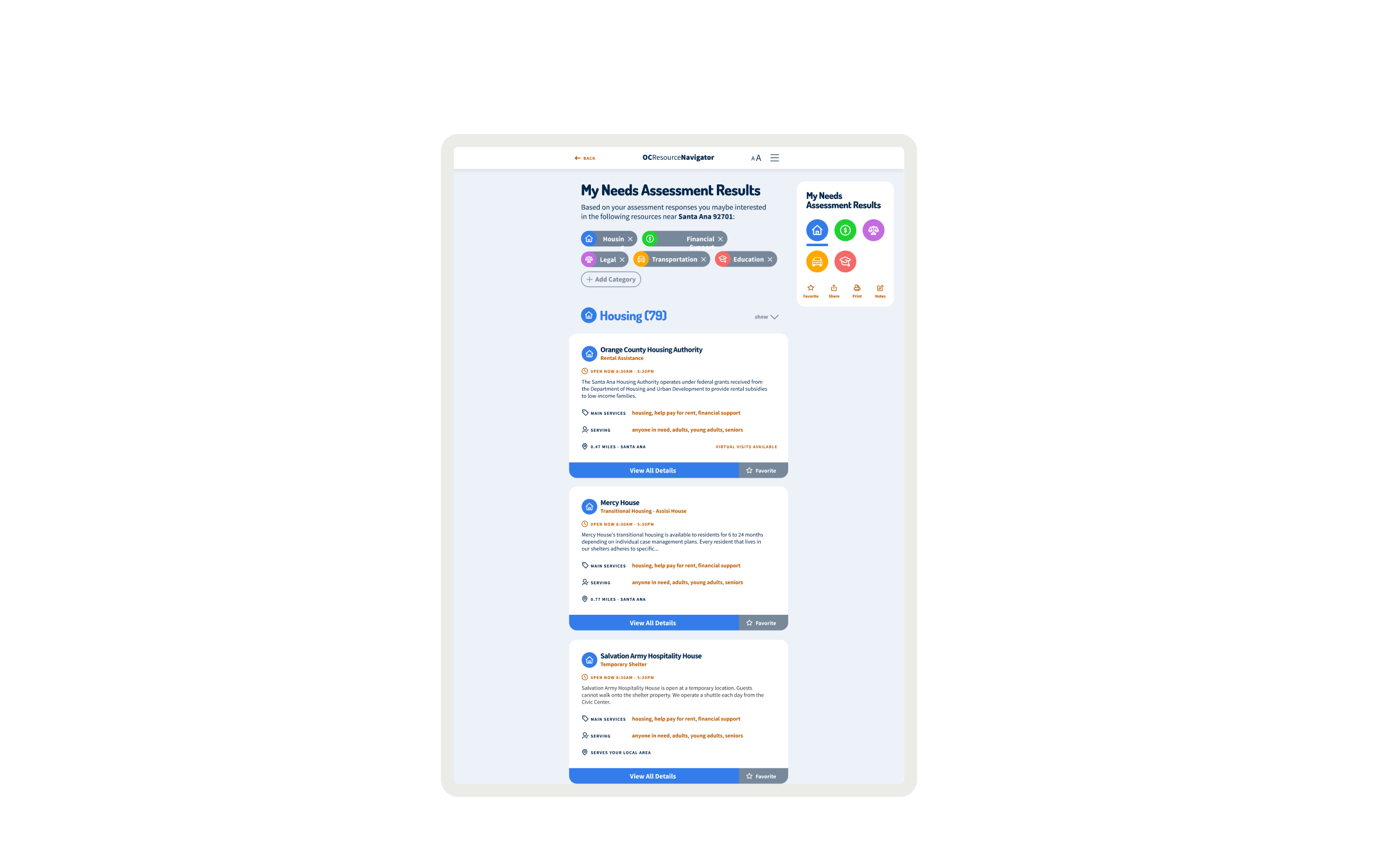
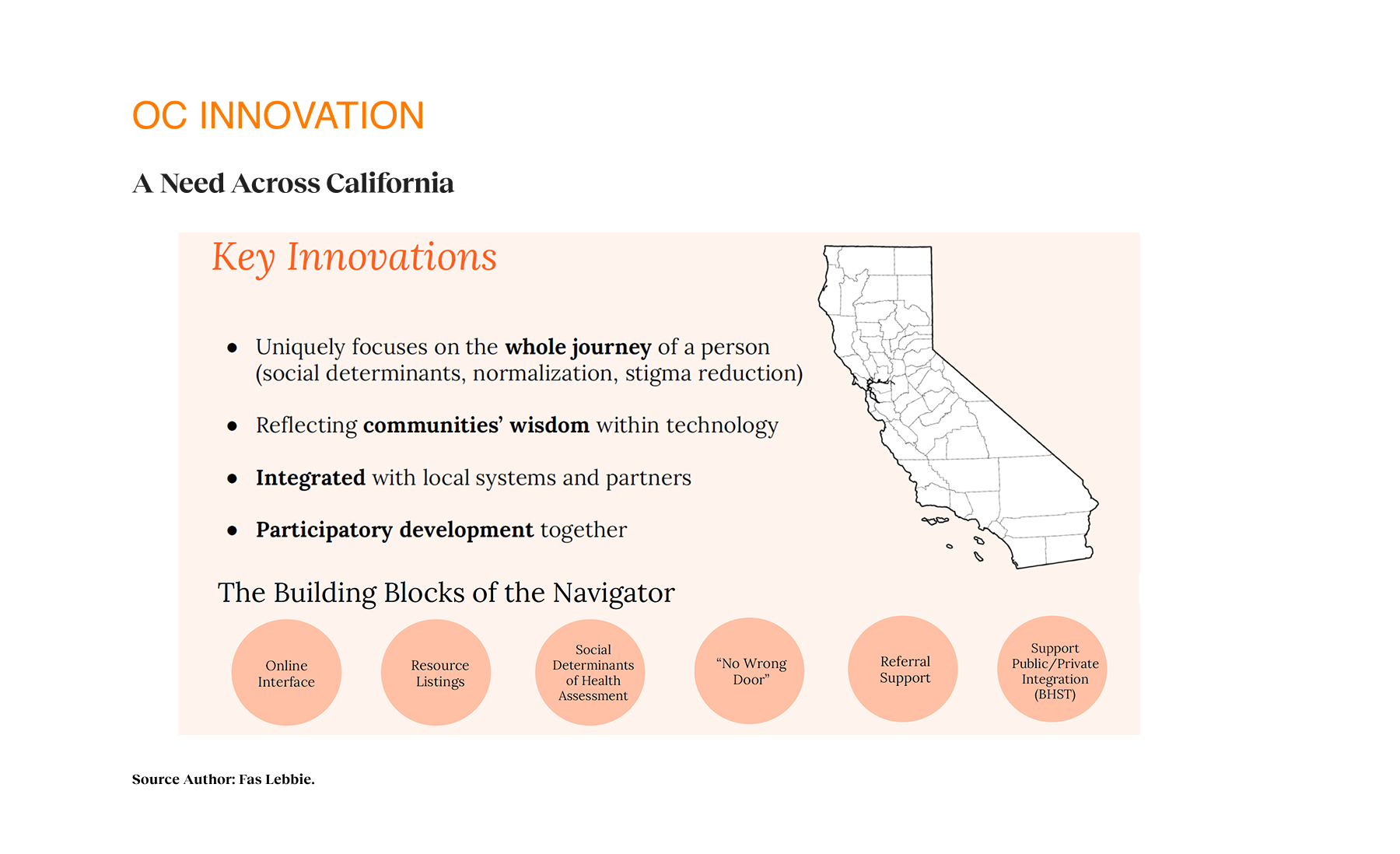
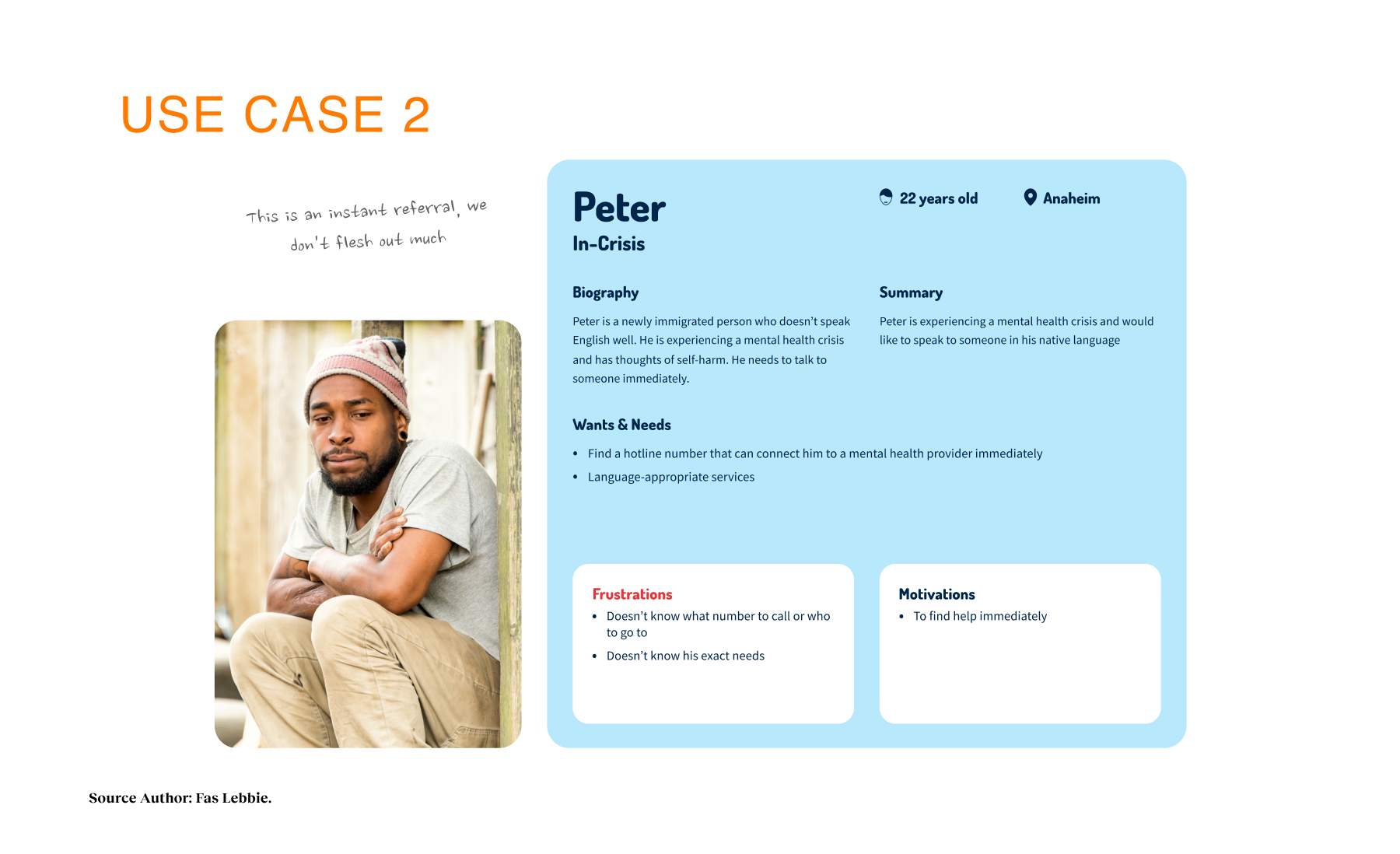
Within the alpha phase, providers described how the tool supported clients in crisis, individuals found previously unknown services, and community organizations saw increased appropriate referrals. The initial resource categories expanded essential areas: housing, financial support, mental wellness, and food security. The design intervention focuses on a person’s whole journey rather than isolated touchpoints. This new system reflects communities’ wisdom, integrates local systems and partners, and uses participatory development. These principles yielded a platform addressing practical needs and emotional barriers to seeking help, normalizing the process of seeking support. By incorporating the social determinants of health screening into navigation, we’re shifting how the mental health system considers comprehensive care. The platform provides a foundation for greater interagency collaboration and data-informed resource allocation as part of the Behavioral Health System Transformation initiative, which addresses a universal need for coordinated mental health resource navigation that transcends geographic boundaries. As adoption increases across Orange County, the project can transform fragmented services into a coordinated system of care.
Next Steps
- Expand Provider Dashboard with referral tracking and outcome measurement to improve accountability and service follow-through.
- Integrate with Health Records for seamless coordination between county systems and providers.
- Develop Culturally Responsive Access by adding a Spanish-language interface and tailored resource categories.
- Create a Mobile App for Accessibility optimized for offline use in low-connectivity areas.